Read time: 5 minutes
Community oncology plays a critical role in improving cancer patient outcomes today. In fact, more than 50% of patients with cancer are treated in a community oncology setting. Not only do these practices provide affordable, state-of-the-art care to patients, but they do so close to patients’ homes – and to their families and support systems.
But the landscape for community oncology is rapidly evolving, driven in large part by COVID-19, growing demand for consumer-facing digital health solutions, a booming oncology drug pipeline and the increased application of precision medicine.
Below, we explore a few of the top trends impacting the future of community oncology, and how McKesson is helping these critical sites of care succeed in the years to come.
Lasting Impact of COVID-19
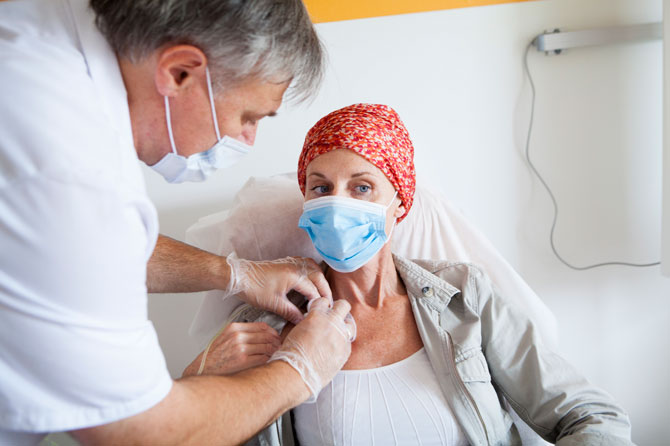
The disruption caused by COVID-19 has been felt in just about every corner of healthcare, and community oncology has not been spared.
One area especially hard-hit was cancer screenings. Many patients have opted to skip routine screenings due to a mix of exposure fears and widespread financial stressors. Additionally, staffing and personal protective equipment (PPE) shortages in the pandemic’s early days forced many hospitals to either shut down or delay screenings for several months. Consequently, fewer screenings resulted in a 13-23% decline in new cancer diagnoses during 2020.
But despite disruption to the patient’s cancer care journey, community oncologists found ways to continue providing quality care when patients most needed it.
“While many hospitals struggled early on to care for ill patients, we saw community oncology practices really stand up and stay open to provide cancer care,” says Marcus Neubauer, MD, chief medical officer for The US Oncology Network (The Network), an organization supported by McKesson with more than 1,400 independent community physicians “Practices across The Network initially focused on maintaining patient access. But over time, community oncology practices found ways to enhance patient care through extraordinary times.”
One of the most impactful shifts COVID-19 has created, Dr. Neubauer explains, has been a more consumer-focused approach to care – one that meets patients where they feel most comfortable. And that’s been made possible through increased technology adoption, particularly in telemedicine.
McKesson has What it Takes to support every aspect of cancer care. See how our unmatched suite of oncology businesses helps enhance the lives of patients living with cancer.
Growing Demand for Telemedicine Services

Prior to the COVID-19 pandemic, many digital health solutions were slow to adoption. But because community oncology practices see some of the most vulnerable patients in the country, telemedicine that enables remote care has been widely implemented across community practices throughout the pandemic to achieve continuity of care, including across all sites in The Network.
Telemedicine can improve health equity by removing accessibility barriers between physicians and their patients. This is especially true for those living in rural and underserved communities who may live far from their nearest cancer care provider. It allows patients to virtually continue their follow-up appointments and check-ins with their oncologists from the comfort of their own homes, minimizing their risk of exposure.
“At this point, it doesn’t appear COVID-19 is going anywhere anytime soon, but neither is the need for quality care,” Dr. Neubauer says. “That’s forced us to become more patient-focused and think more about how to improve the patient experience through various technologies – not just throughout the pandemic, but beyond as well.”
Booming Precision Medicine Market

One of the most promising evolutions in cancer care has been in the field of precision medicine, an approach in which genomics – along with a patient’s cancer type and their clinical setting – are factored into a patient’s treatment plan.
Rather than taking a one-size-fits-all approach to treatment, precision medicine allows oncologists to identify alterations and mutations in an individual’s cancer so they can better understand its cause and ultimately tailor treatment to that patient and their disease. And while the oncology community has certainly come a long way in its understanding and adoption of precision medicine in recent years, it’s just beginning to scratch the surface, Dr. Neubauer explains.
“We are immersed in the evolving arena of precision medicine,” he says. “Every day, the oncology community is learning more about cancer-causing mutations. The more we know, the more we can target therapies that improve outcomes and minimize unwanted side effects.”
The proliferation of data, evidence and new research means oncologists must stay abreast of developments in therapies, care pathways, diagnostics and more. That’s another place where technology can help. Through the Clear Value Plus clinical decision support tool from Ontada, McKesson’s oncology real-world data and evidence, clinical education and provider technology business, oncologists can view evidence-based treatment options matched to each patient, while providing integrated clinical and financial information at the point of need.
Tapping into Real-World Data to Advance Precision Medicine
If patients carry the same mutation for a certain type of cancer, how can oncologists provide better care to people with that mutation?
One way to examine outcomes of targeted therapies is by using real-world data (RWD). RWD is data that relates to a patient’s health status or delivery of care, which is routinely collected from a variety of sources during the course of a patient’s treatment, such as diagnosis, disease stage and progression, treatment, and any reactions to their therapies. Using an electronic health record (EHR), like McKesson’s proprietary iKnowMedSM, Ontada can gather the anonymized records of patients with similar cancers sharing the same mutation and examine their response to a particular therapy.
“The Network sees over a million patients every year,” explains Nicholas Robert, MD, chief medical officer for Ontada. “Using the data gathered in iKnowMed, we can create databases around certain biomarkers including mutations from patients across community oncology sites. This presents an excellent opportunity for us to lead the way in supporting better patient care and advancing research.”
What’s ahead
The pace of change may be quickly accelerating, but McKesson is well-positioned to guide and support patients and providers into this new era of community oncology.
“The complexity of running a community oncology practice and providing optimal cancer care is greater than ever before,” explains Heather Morel, president of Provider Solutions for McKesson. “We believe we are uniquely positioned to help our partners through these challenges – from our practice management leadership through The Network to proprietary technologies like iKnowMed, to Ontada’s data, insights and evidence capabilities. Our goal is to keep community oncology flourishing so patients can get quality care close to home.”




Share
Post
Post
Email